Hand eczema, or hand dermatitis, describes any type of eczema that develops on the hands. It is commonly job-related and can be made worse by frequent hand washing and exposure to chemicals. Hand eczema may require specific testing and treatment. It may cause itchy, dry, scaly skin that cracks and flakes. Hand eczema can be mild, moderate, or severe, and more severe forms of the condition can be extremely painful and debilitating.
According to recent evidence, the annual prevalence of chronic hand eczema in adults in Canada is 6.2% (Apfelberger C et al, 2025).¹
Moisturizing the skin and using gentle cleansers are the first defence against hand eczema. Apply a rich moisturizer immediately after hand washing, bathing, wet work, and anytime in between.
Internal and External Triggers of Hand Eczema
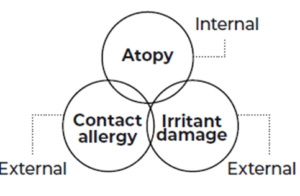
Atopy – an impaired skin barrier and immune system prone to atopic eczema contributes to hand eczema.
Contact allergy – coming in contact with an allergy can trigger a flare and can trigger hand eczema.
Exposure to irritants – coming in contact with irritants can trigger a flare and can trigger hand eczema.
To treat inflammation, there are topical medications, including creams or ointments that can be used to treat hand eczema. These include topical corticosteroids, and a newer class of medication called topical JAK inhibitors.
Topical corticosteroids are commonly used. These should be used only as needed — that is, when your eczema is actively flaring. Prolonged use of topical corticosteroids can cause side effects such as thinning of the skin. If your response is unexpectedly slow, although it is rare, discuss the possibility of corticosteroid allergy with your doctor.
Narrow-band UVB light and PUVA are helpful for their local immunomodulatory effect. Speak to your doctor about the possibility of phototherapy as a treatment option. There are specific Phototherapy units that are used to treat the hands.
Oral corticosteroids may be effective in a short course for recurrent pompholyx and dyshidrotic hand dermatitis, however, should be avoided and used only for severe flare-ups. Patients need to be aware of the serious side effects of oral prednisone.
Alitretinoin (e.g. Hanzema™, Toctino®) is an oral retinoid. A once-daily treatment, it is available for patients suffering from severe symptoms that never go away completely or keep coming back even after using potent topical steroids. Research has demonstrated significant clinical improvement in patients with chronic hand eczema, especially for the variant known as hyperkeratotic dermatitis. Side effects include headache and flushing. Some patients are not suitable candidates for alitretinoin. Speak with your doctor about this treatment.
IMPORTANT NOTE: Strict pregnancy prevention is required 1 month before, during, and for 1 month after treatment with alitretinoin for women of child-bearing potential due to the teratogenicity of the product (the product can cause birth defects). Never share your prescription of alitretinoin and speak with your doctor about whether this treatment is right for you.